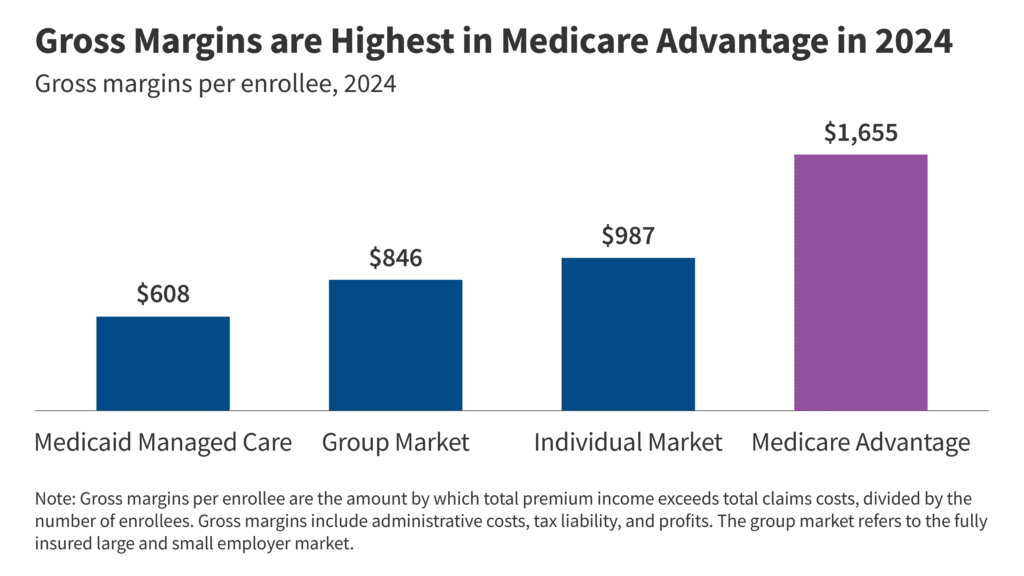
Individual Market: The individual market includes coverage purchased by individuals and families through the Affordable Care Act’s exchanges (Marketplaces) as well as coverage purchased directly off-exchange, which includes both plans complying with the ACA’s rules and non-compliant coverage (e.g., grandfathered policies purchased before the ACA went into effect and some short-term plans). The federal government provided subsidies for low and middle-income people in the Marketplace and includes measures, such as risk adjustment, to help limit the financial liability of insurers. Insurers in the individual market receive premium payments from enrollees, plus any federal subsidies for people in the Marketplaces.
Some plans submitting data on the Exhibit of Premiums Enrollment and Utilization appear to be including some Children’s Health Insurance Program (CHIP) data in their Individual market filings. In a previous version of this analysis, we used the Supplemental Health Care Exhibit to address this. However, in this analysis, we opted to use the EPEU to ensure comparability.
Group Market: The fully insured group market serves employers, their employees and dependents who are enrolled in fully insured health plans. This market includes both small and large group plans but excludes employer-sponsored insurance plans that are self-funded, which account for 63% of workers with employer-sponsored insurance in 2024. This analysis does not capture metrics for the Federal Employee Health Benefit Program or California Managed Health Care plans. Roughly 25 million people from the fully insured group market in 2024 are accounted for in this analysis. Plans typically receive premium payments from both employers and their employees.
Medicaid Managed Care: The Medicaid managed care market includes managed care organizations (MCOs) that contract with state Medicaid programs to deliver comprehensive acute care (i.e., most physician and hospital services) to enrollees. As of July 2024, more than three-fourths (over 66 million people) of all Medicaid beneficiaries nationally received most or all of their care from comprehensive risk-based MCOs. There is significant variation across states with respect to services that are covered by MCOs.
In this analysis, the NAIC data we use defines “Medicaid” as “business where the reporting entity charges a premium and agrees to cover the full medical costs of Medicaid subscribers” and only explicitly excludes Administrative Services Only (ASO) plans from their reporting. While we only use “medically” focused plans to help exclude any specialty plans, PAHPs, PIHPs and PACE plans may not be excluded due to NAIC’s definition of Medicaid. Additionally, for Medicaid, there are four states (California, Delaware, New York, and Oregon) that have different reporting practices and therefore may only have partial or no NAIC data available for the years displayed. In other work, KFF defines comprehensive MCOs as managed care plans that provide comprehensive Medicaid acute care services and, in some cases, long-term services and supports as well. This excludes “limited benefit plans” including prepaid ambulatory health plans (PAHPs), prepaid inpatient health plans (PIHPs), and Programs of All-Inclusive Care for the Elderly (PACE) that may be included in this analysis.
Medicare Advantage: The Medicare Advantage market provides Medicare-covered benefits through private plans to around 33 million Medicare beneficiaries in 2024, which is over half of all Medicare beneficiaries in 2024. The federal government makes risk-adjusted payments (higher payments for sicker enrollees and lower payments for healthier enrollees) to plans (averaging nearly $14,823 per enrollee in 2024) to cover the cost of benefits covered under Medicare Parts A and B and supplemental benefits, such as dental, vision, hearing, and others, with additional payments for costs associated with prescription drug coverage. Some plans charge enrollees an additional premium.