As the latest KFF Health Tracking Poll shows, affordability is the public’s biggest concern, with the cost of health care ranking as their top economic worry. However, KFF polls have demonstrated that beyond costs, insured people report a whole host of issues navigating the health care system. This report looks at which aspects of accessing care and health insurance are the biggest problem for insured adults and finds that prior authorizations – or the process of having to get insurance approval before accessing certain tests, treatments, or medications – are having an outsized impact on insured adults.
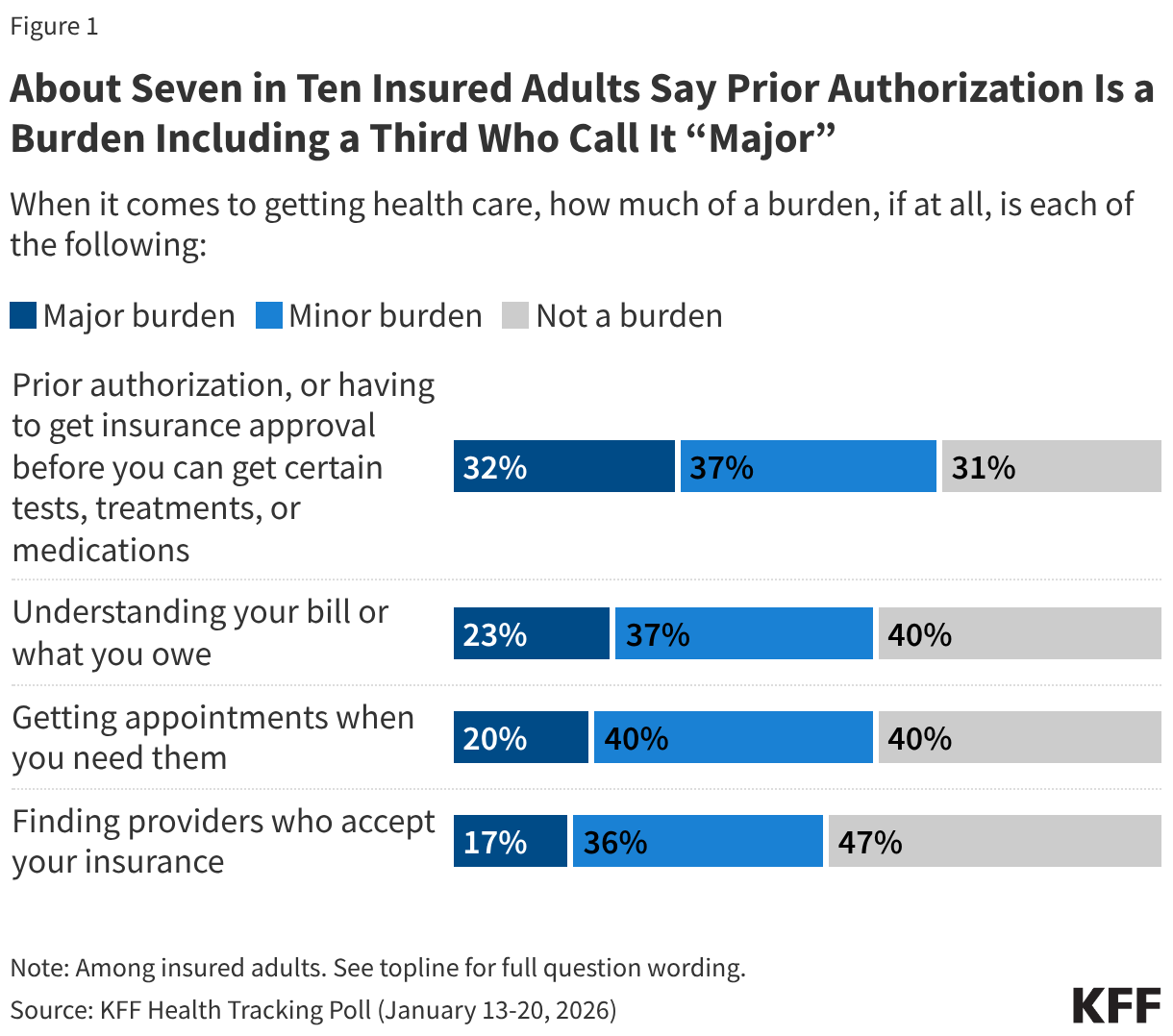
One in three insured adults in the U.S. say they find prior authorizations a “major burden” to getting health care. An additional four in ten (37%) say the process is a “minor burden,” bringing the total share of insured adults who find the process burdensome to about seven in ten (69%). This is larger than the share who say other aspects are burdensome such as understanding bills or what is owed (60%), getting needed appointments (60%), or finding providers who accept their insurance (53%).
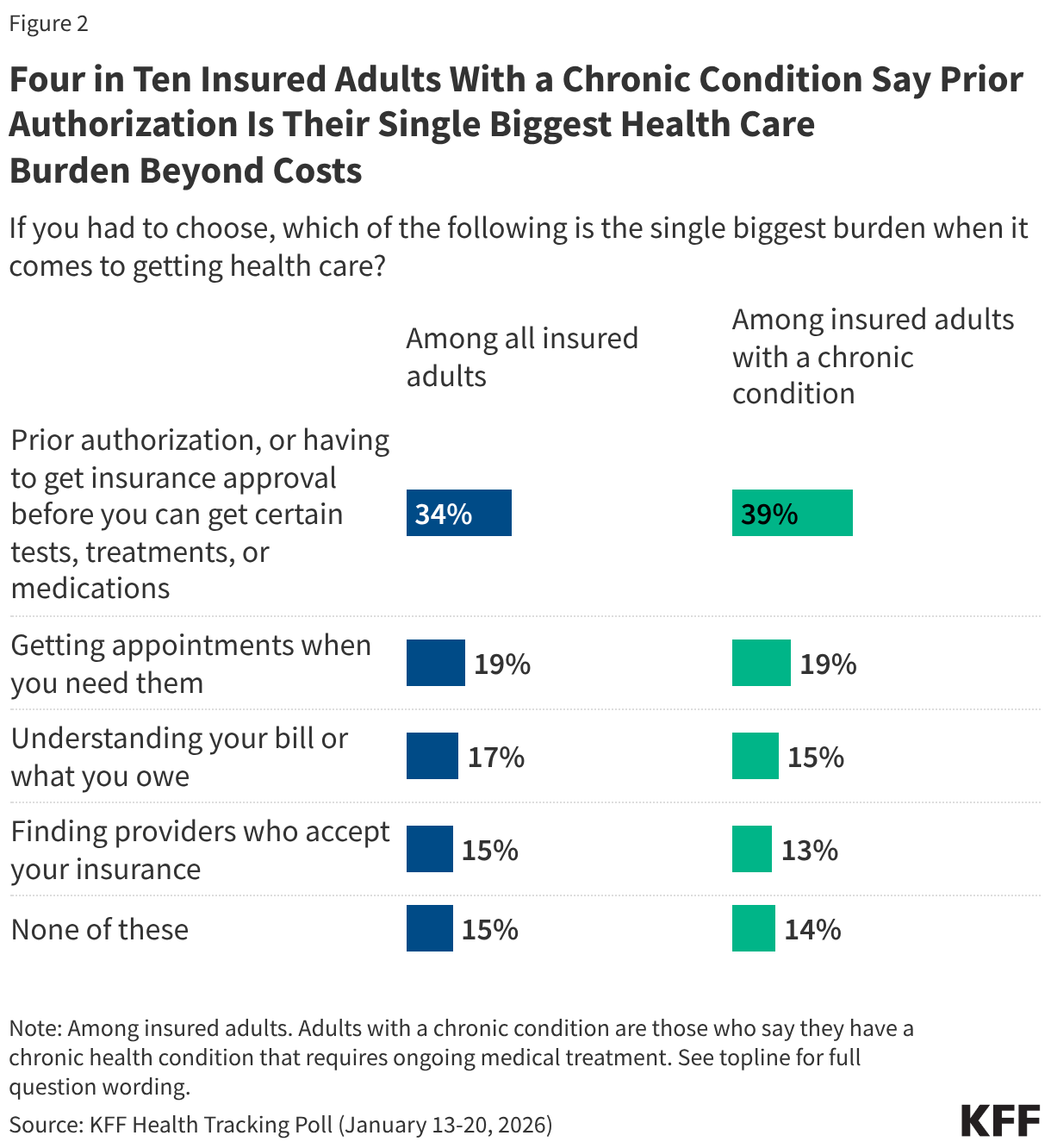
When asked to choose which aspect of getting health care, beyond costs, is the single biggest burden, one in three insured adults (34%) choose prior authorizations, followed by getting needed appointments (19%), understanding their bill (17%), or finding providers who accept their insurance (15%). The choice of prior authorizations as the single biggest burden is even more stark among adults with a chronic condition that requires ongoing medical treatment (about half of all adults). These individuals often require more treatments and medications, resulting in more interactions with health insurance companies and health care providers. Four in ten (39%) insured adults with a chronic condition say prior authorizations are the single biggest burden when it comes to getting health care, at least twice the share who say the same about the other aspects of health care asked about.
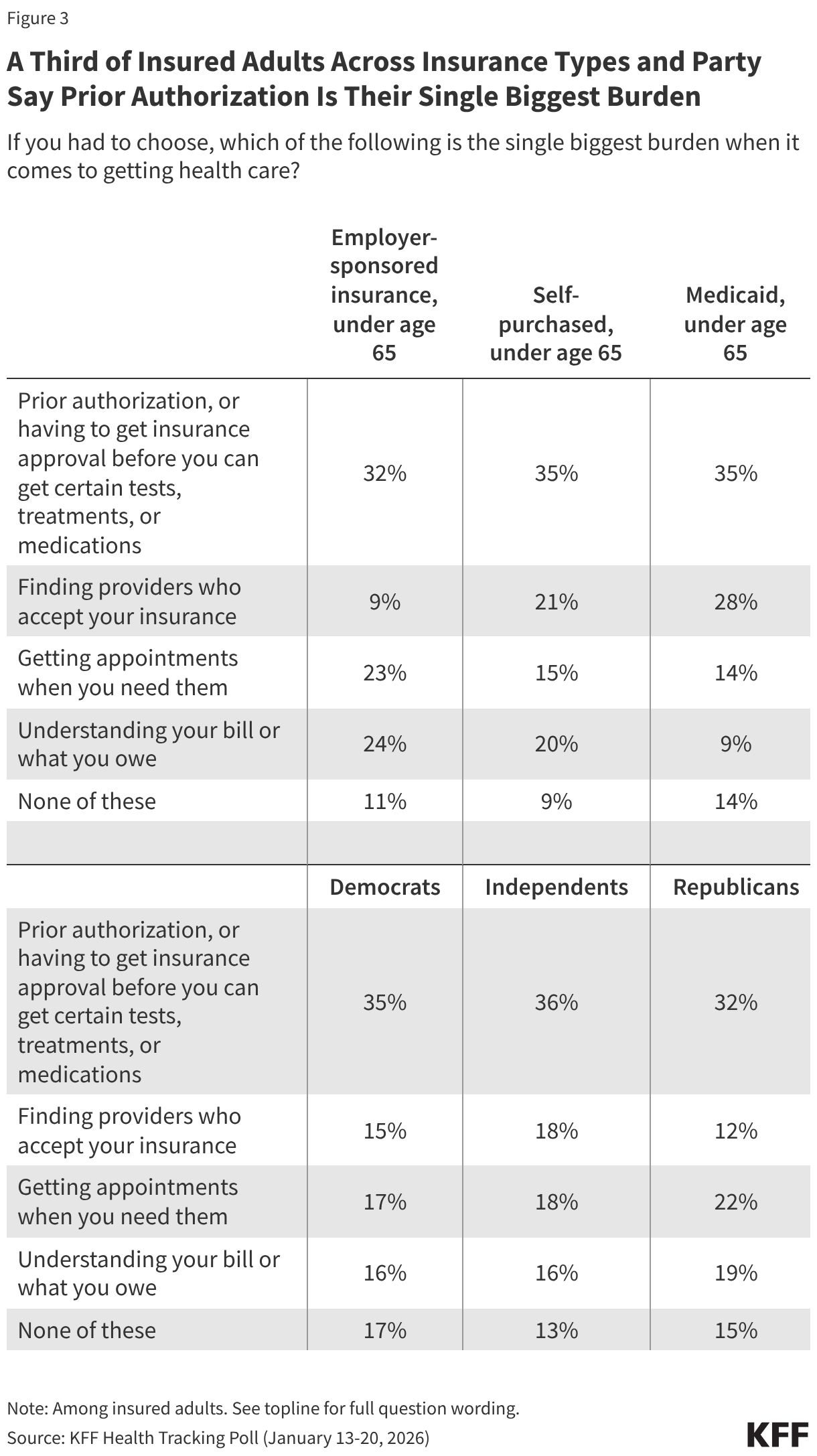
Prior authorizations are also identified as the single biggest burden for insured adults across partisans, as well as among individuals across insurance types that typically require prior authorizations such as individuals with Medicaid, people who buy their own health insurance, and people who get health insurance through an employer. Notably, about three in ten (28%) Medicaid enrollees identify finding providers who accept their insurance as the biggest burden, but small shares identify other issues as their biggest burden.1
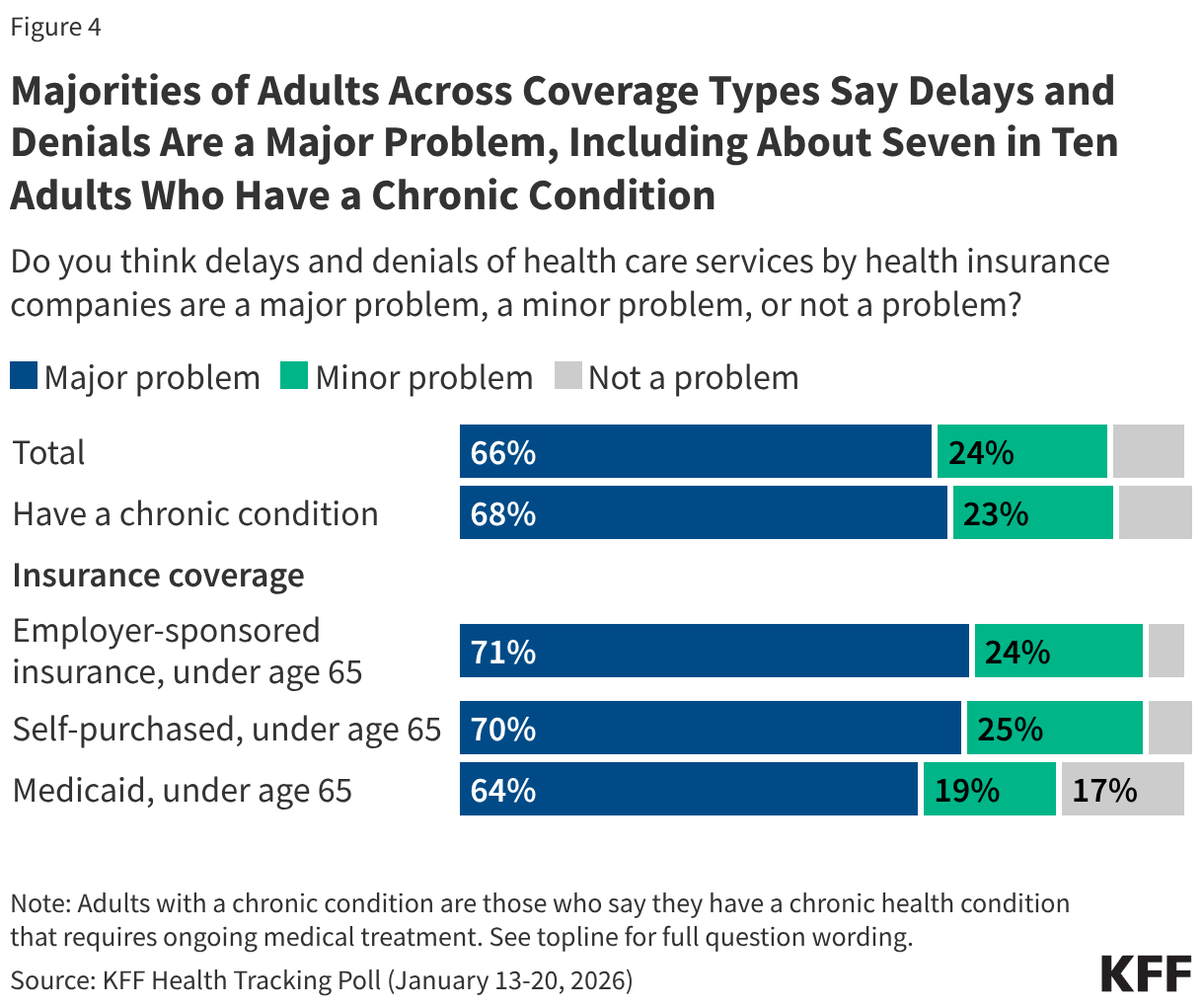
During the prior authorization process, some treatments or medications recommended by a provider may be delayed and, in some instances, an insurance company may end up denying medication or treatment. Overall, about two-thirds of adults say delays and denials of health care services by health insurance companies are a “major problem” with an additional one in four (24%) who say they are a “minor problem.” Just one in ten adults say delays and denials of services by insurance companies are not a problem in our current health care system. More than six in ten across Medicaid enrollees, self-purchasers, and those with employer coverage say the delays and denials of care by insurance companies are a “major problem.”
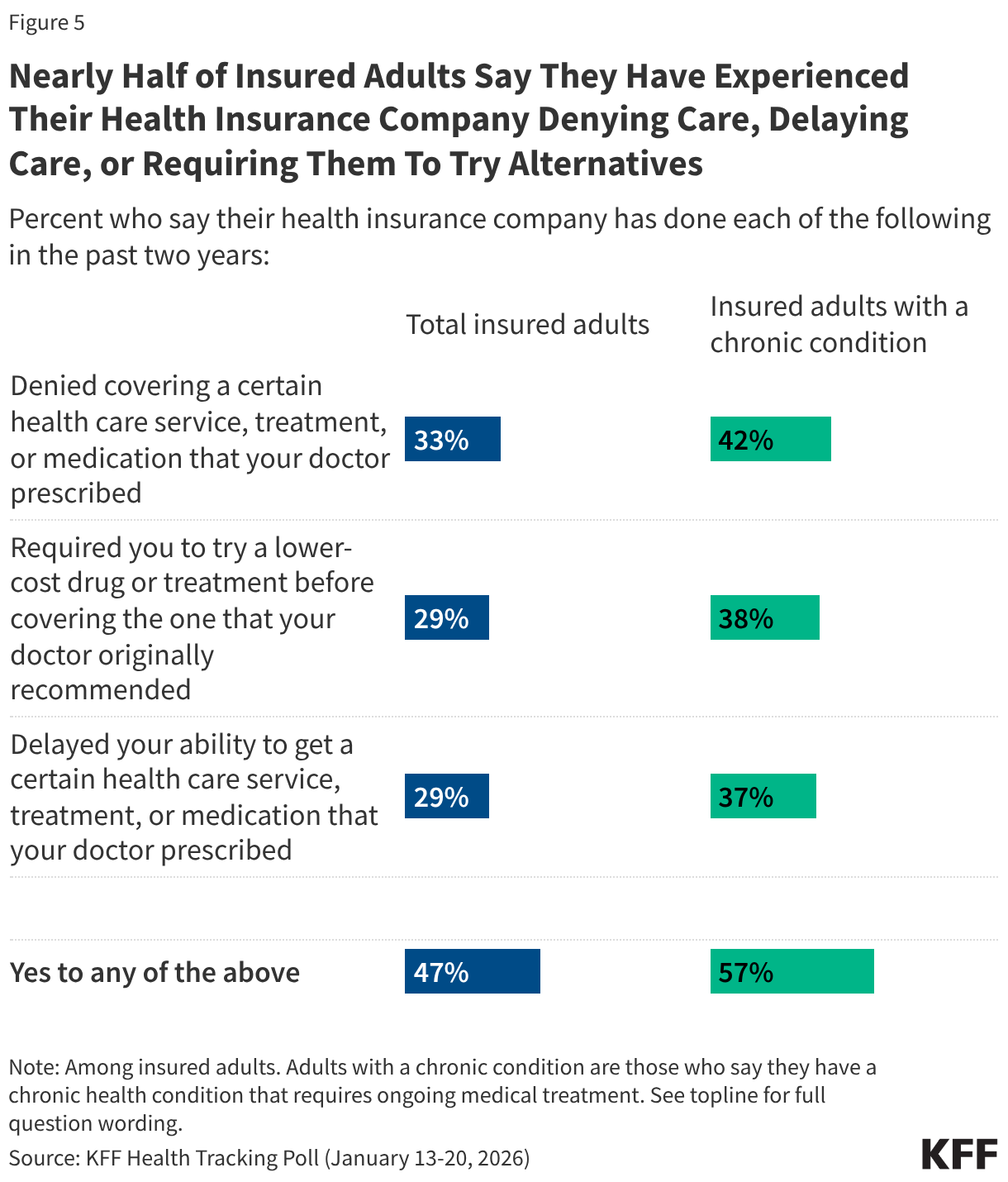
About one in three insured adults (33%) say they have had a health insurance company deny coverage for a certain health care service treatment, or medication prescribed by their doctor in the past two years. Three in ten insured adults say that a health insurance company has delayed their ability to get such services, treatments, or medications (29%) or required them to try a lower-cost drug or treatment before covering the one that was originally recommended by their provider (29%). These issues are even more common among insured adults with a chronic condition with about four in ten reporting that an insurance company has required them to try a lower-cost drug or treatment (38%), deny coverage for a certain service or medication (42%), or delayed their ability to get prescribed care (37%). Overall, nearly half (47%) of insured adults say they have had a certain service, treatment, or medication either denied or delayed in the past two years, rising to nearly six in ten (57%) among those with a chronic condition.
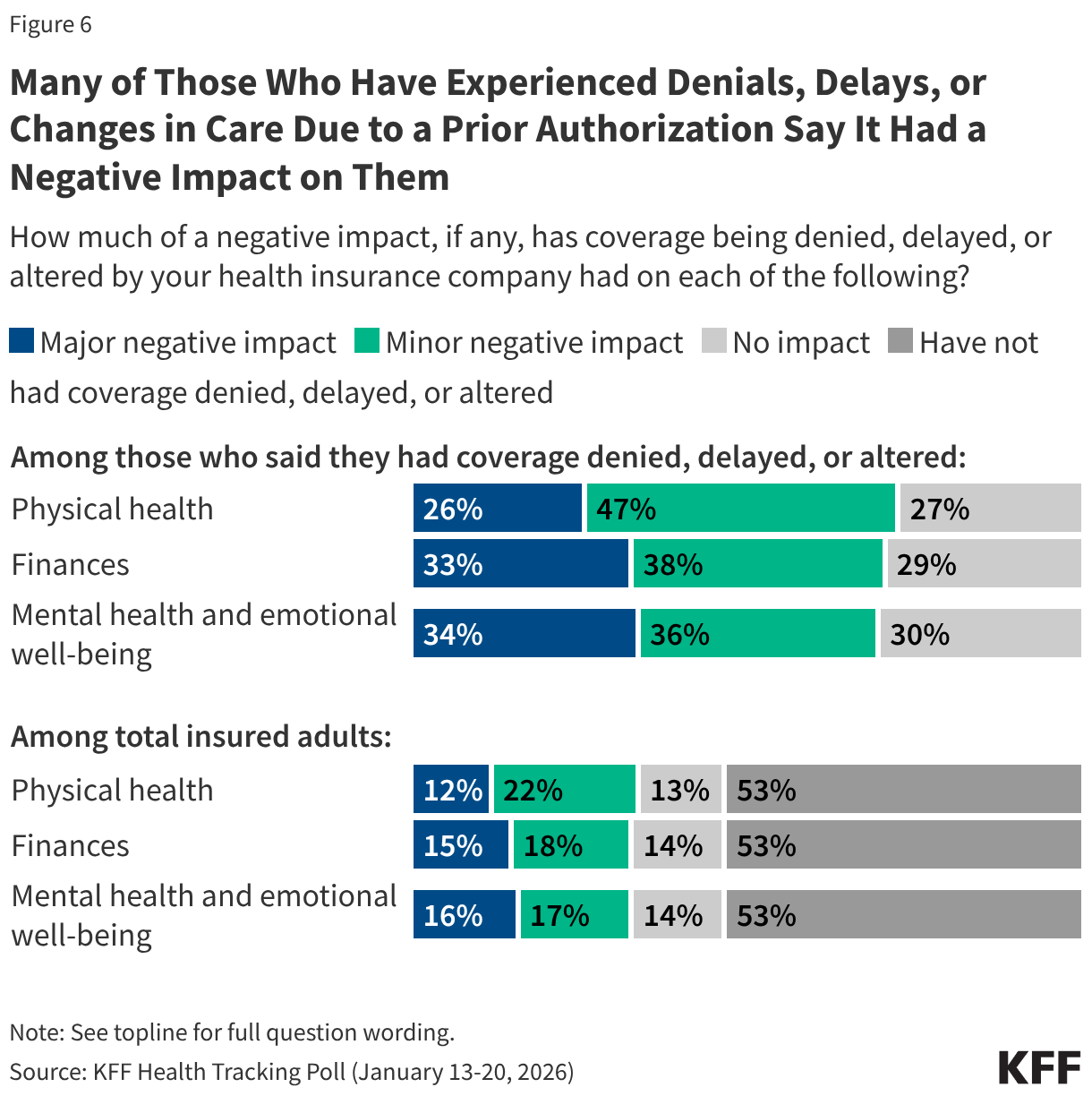
Denial and delays by health insurance companies can lead to negative consequences for people’s physical, mental, and financial health. One in three of those who experienced a denial or delay say the actions required by their health insurance company had a “major negative impact” on their mental health and emotional well-being as well as on their finances (about one in six of all insured adults). One in four (one in eight of all insured adults) say the delays or denials has a “major negative impact” on their physical health.