Judging by more than 16,400 comments recently posted on a federal government website, you’d think there was a groundswell of older Americans demanding that federal officials hike payments to their Medicare Advantage health insurance plans.
Yet about 82% of the comments are identical to a letter that appeared on the website of a secretive advocacy group called Medicare Advantage Majority, a data analysis by KFF Health News has found.
The “dark money” group does not reveal its funders or much else — other than to say it is “dedicated to protecting and strengthening Medicare Advantage” and is “powered by hundreds of thousands of local advocates nationwide.”
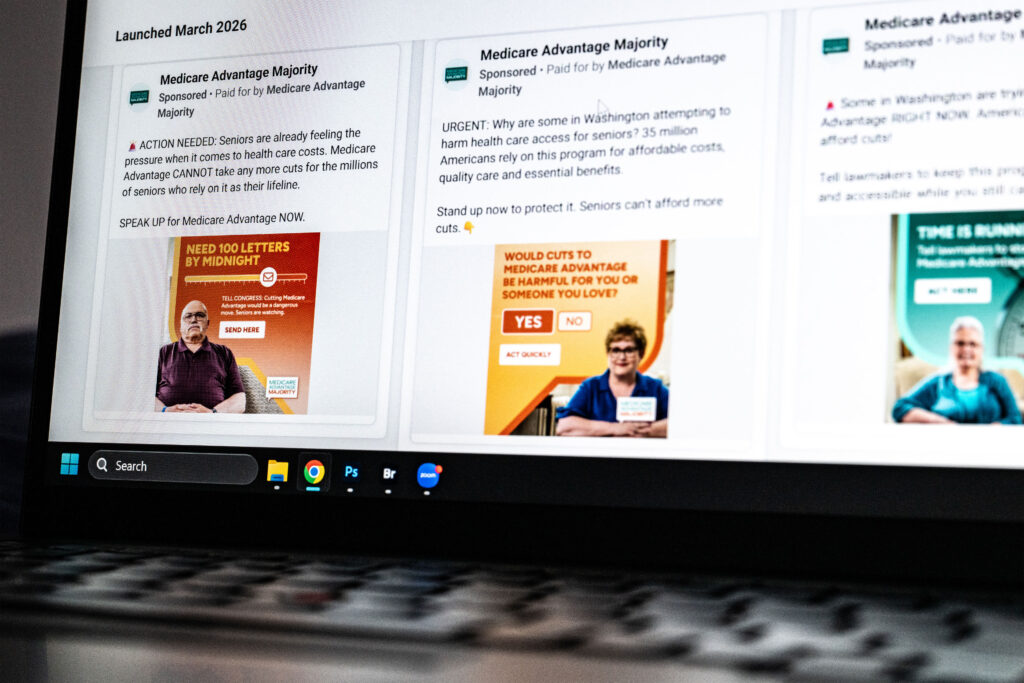
“Our campaign provides information and offers tools for concerned Americans to use to reach decision makers,” spokesperson Darren Grubb said in an email. The group has spent more than $3.1 million on hundreds of Facebook ads since September 2024, according to Facebook’s Ad Library, a database of the social media company’s online ads.
There’s no doubt health insurers are unhappy with a January proposal from the Centers for Medicare & Medicaid Services, or CMS, to keep Medicare Advantage reimbursement rates essentially flat in 2027 — far less than they expected from the Trump administration.
Medicare Advantage plans differ from traditional Medicare because private insurance companies administer them. The insurance plans enroll about 35 million members, more than half the people eligible for Medicare. The plans offer things like vision and drug coverage, but Medicare Advantage insurers restrict the hospitals and doctors that patients can use and require prior approval for various procedures.
CMS is set to announce a final decision by early next month on the rate proposal. The agency solicited public comments on the proposal from Jan. 26 through Feb. 25 to give interested parties and the public a chance to air their views.
Medicare Advantage Majority, which says the rate proposal amounts to a “cut” in services and warns of dire consequences for seniors should it go through, accounted for at least 13,522 of the 16,422 comments published as of March 12.
The proposed rate plan “puts my access to care at risk,” the group’s template letter to policymakers reads in part. “If the investment made by Washington in the Medicare Advantage program is nearly flat year-over-year, I could lose benefits I rely on every day, including affordable prescriptions, capped out of pocket costs, and access to trusted doctors and specialists.”
“Medicare Advantage is not optional for me. The cost protections alone have saved me thousands of dollars and made my health care manageable. Without this program, I would face higher costs, fewer providers, and fewer benefits at a time when I can least afford it,” the letter states.
Critics warn that these sorts of campaigns may create a misleading impression of grassroots support, especially when it’s not clear who is financing them.
“It puts a different spin on a massive groundswell of comments to know all are being driven by one specific organization,” said Michael Beckel, director of money in politics reform for Issue One, a group that seeks to limit the influence of money on government policy and legislation.
“There’s no way for the public to know what wealthy donors or special interests are funding dark money groups like this,” he said. “That means there’s no scrutiny of who’s really calling the shots.”
Some health care policy experts, who have long argued that the government overpays Medicare Advantage plans by tens of billions of dollars every year, believe industry groups or their surrogates routinely overstate possible negative impacts of rate decisions they don’t like.
“The plans always say that the sky is falling,” said Matthew Fiedler, a health care policy expert with the Brookings Institution. “The industry has a lot of money at stake here. They try to exert pressure on policymakers any way they can.”
At the same time, even critics concede that some of the millions of people enrolled in Medicare Advantage plans could face service cuts if insurance companies are not satisfied with government payments.
“It is legitimate for people to be worried,” said Julie Carter, counsel for federal policy at the Medicare Rights Center, a group that advocates for older adults and people with disabilities.
Her group argues that Medicare Advantage plans have never attained expected cost savings and instead have been overpaid for years at least partly due to “actions to maximize profits.” She said the health plans “are supposed to be saving money, not taking extra.”
People struggling to pay health care bills may have little use for the policy debate in Washington.
“If it wasn’t for being able to have this program, I really wouldn’t be able to afford any kind of medical services, to be honest,” said EsterAlicia Rose, 75, who works at the front desk of a hotel in Pagosa Springs, Colorado. She said she signed the Medicare Advantage Majority form letter to reach policymakers.
Kathy Lovely-Marshall, 66, a retired nurse who lives in Brookville, Ohio, did too. She said she receives “a lot of perks” from her plan, such as dental care, eyeglasses, and prescriptions.
“All those things are a big plus as far as I am concerned,” she said. “I’m very happy with the plan I have.”
But Corenia Branham, 90, a widow and cancer survivor who lives in Alum Creek, West Virginia, said she wants nothing to do with Medicare Advantage plans run by private health insurance companies. She said she didn’t turn in any of the four form letters under her name, which were posted online by CMS on Feb. 23 and signed, “Miss Corenia Branham Branham.” It’s not clear why her last name is signed twice.
Branham said she’s not on Medicare Advantage and doubts she could count on it for needed care.
“I wouldn’t recommend it to nobody,” she said. “I sure don’t want anything to do with it.”
Grubb, the Medicare Advantage Majority spokesperson, disputed that account. He said Branham responded to an ad on Facebook. On Feb. 6, she “completed the form with her information and chose to send her comment to CMS as well as to her representatives in Congress and the White House,” he said.
Other Medicare Advantage advocacy groups have stepped up ad campaigns as the rate decision looms.
The Better Medicare Alliance, whose “allies” include a range of health insurers, health care providers, and consumers, is urging seniors to “Tell Washington to Stand Up for Medicare Advantage.”
“We’ve mobilized beneficiaries to write letters and make phone calls, and we’ve run digital ads on streaming platforms,” spokesperson Susan Reilly said.
Reilly said that this year roughly 3 million seniors “were forced to find new coverage” because plans either shuttered operations or left some areas.
She also said Medicare Advantage plans have “scaled back” benefits such as offering transportation to medical appointments, nutrition support, and dental and vision coverage, while over the past two years beneficiaries have faced an average $900 increase in out-of-pocket maximums.
“We do view this as especially serious,” Reilly said. “This isn’t a single bad year; it’s the cumulative effect of years of underfunding and policy disruption from the previous administration that has left the program increasingly vulnerable.”
As of March 12, CMS said it had received 46,884 comments but had posted only 16,422 online.
CMS spokesperson Catherine Howden said the agency would make more comments public “as soon as practicable.”
“The agency focuses on reviewing the substance of timely submissions and does not speculate on volume, sentiment, or potential impact of comments while the comment period is open/under review,” she said in a statement.