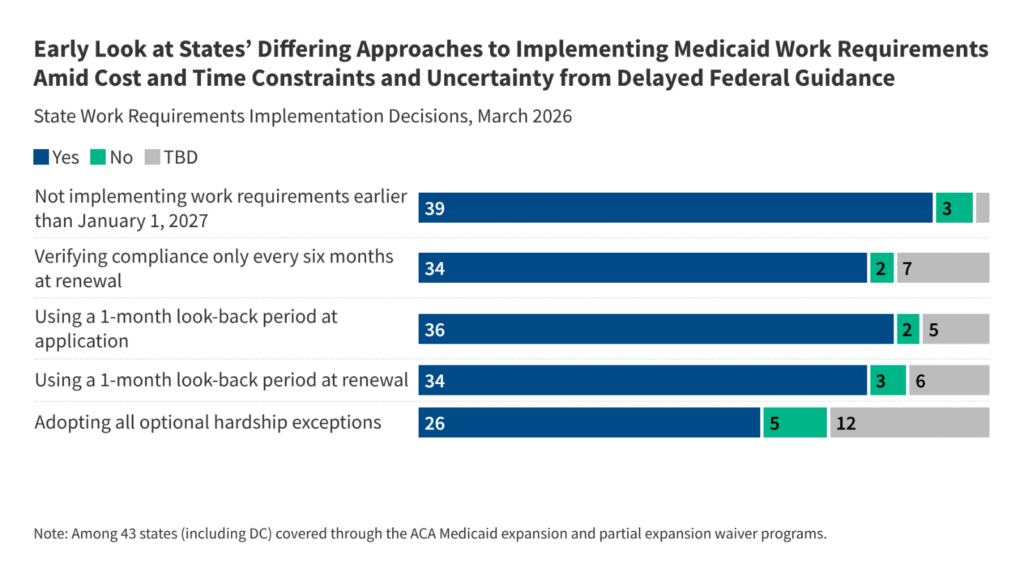
State Decisions on Implementation Timing, Compliance Verification, and Hardship Exceptions
Implementation Timing
Most states are planning to implement work requirements on January 1, 2027, as required by the law; however, three states indicated they will implement earlier. The 2025 reconciliation law requires states to implement work requirements starting January 1, 2027. States have the option to implement requirements sooner through a state plan amendment or through an approved 1115 waiver. Nebraska was the first state to announce that it would begin enforcing Medicaid work requirements early, starting May 1, 2026. Montana has indicated it will begin enforcing work requirements on July 1, 2026, and Iowa will implement on December 1, 2026. In one additional state, Kentucky, a final decision on implementation date had not been made at the time the survey was fielded. Arkansas recently announced that it will launch a soft implementation of work requirements. Starting July 1, 2026, the state will begin checking whether enrollees meet the new requirements or qualify for an exemption. The state will notify individuals of their status but will not disenroll anyone who does not meet the requirements until January 2027.
Verification Frequency and Lookback Periods
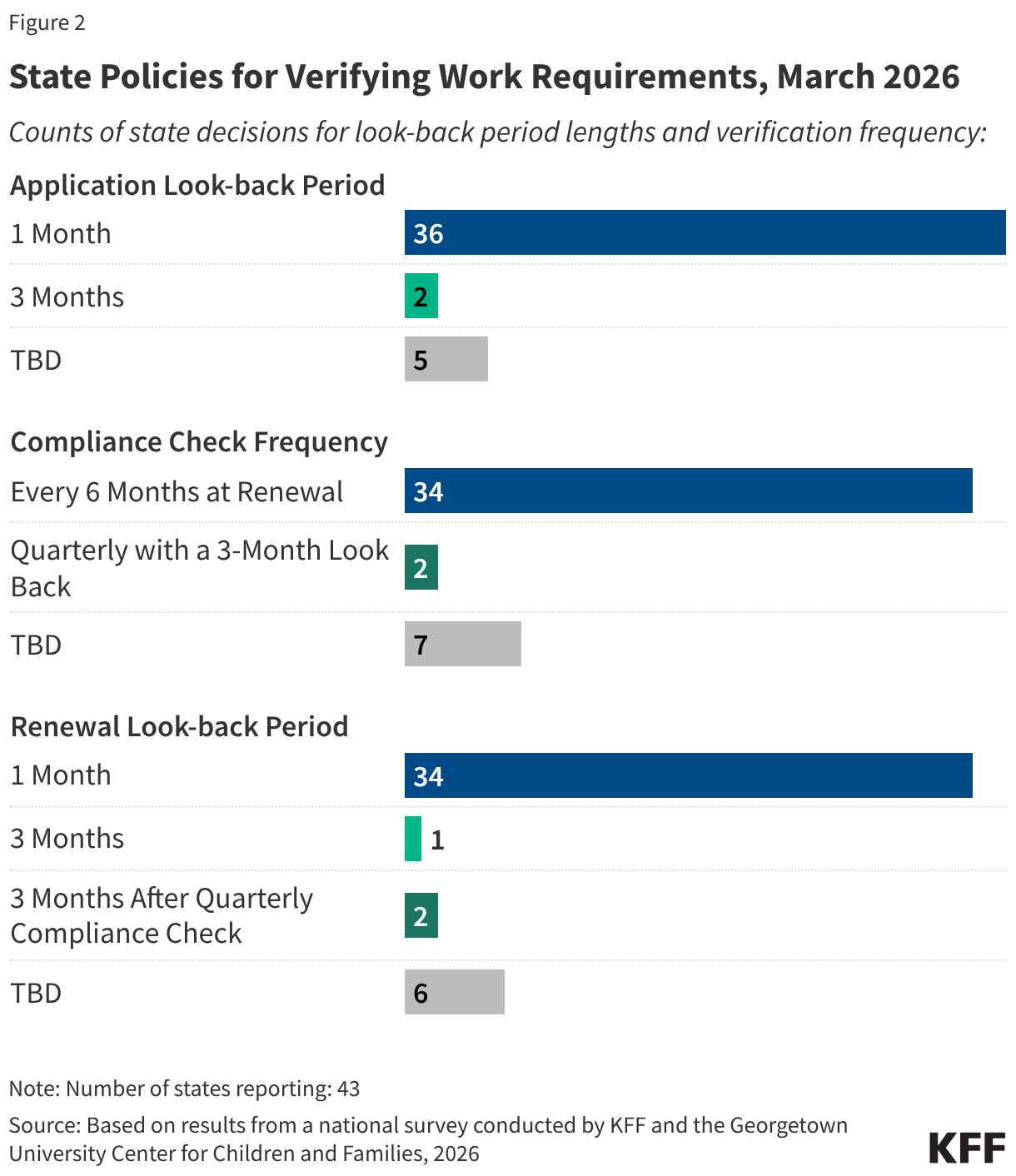
Thirty-four states reported that they will verify compliance with work requirements every six months at renewal, while two states, Indiana and New Hampshire, will verify compliance with work requirements quarterly. The 2025 reconciliation law requires states to confirm individuals are meeting work requirements or are exempt at application and every six months at renewal, but it also gives states the option to verify compliance more frequently between renewal periods. State legislation in both Indiana and New Hampshire requires the Medicaid agencies to conduct quarterly compliance checks. Seven states have not yet made a decision on the frequency of compliance checks (Figure 2).
While the majority of states will implement a one month look back at application and renewal, two states will look back three consecutive months at application while three states will look back more than one month at renewal. At a minimum, states must look back one month immediately preceding the application month and one month between renewal periods to confirm compliance with the requirements. States may impose a longer lookback period, up to three consecutive months at application, and may require compliance in more than one month between the six-month renewal periods. At application, 36 states will look back one month to verify compliance with work requirements or exemption status, and 34 states will look back one month at renewal (Figure 2). Indiana and Idaho will look back three months at application. Indiana and New Hampshire will check quarterly and at renewal to verify that enrollees meet the requirements every month between renewals. Arkansas will also look back three months at renewal but is not planning quarterly checks. States that had not made a decision at the time of the survey included five states for application, six states for renewal, and seven states for more frequent checks.
Optional Hardship Exceptions
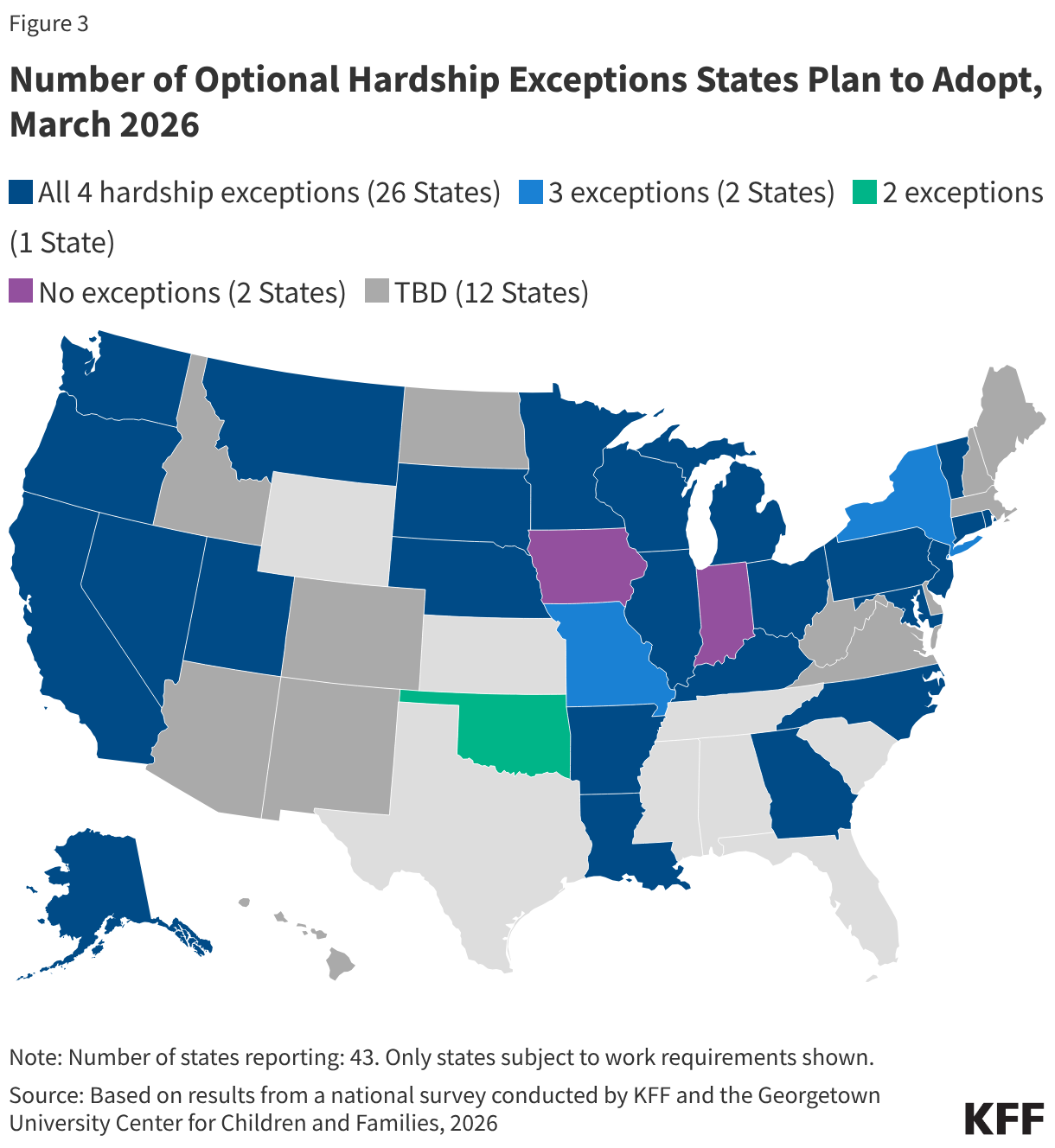
Twenty-nine states reported plans to adopt at least one optional hardship exception, and all but three of those states indicated they will adopt all four exceptions (Figure 3). States are permitted to allow short-term hardship exceptions from work requirements for enrollees (or applicants) experiencing certain extenuating circumstances, including residing in counties with high unemployment rates or experiencing natural disasters, individuals admitted to a hospital or nursing facility, or those who must travel outside of their community for an extended period to obtain medical care for themselves or a dependent. Indiana and Iowa do not plan to adopt any hardship exceptions. Oklahoma is not adopting the exceptions for residents of counties with high unemployment or with a declared natural disaster while Missouri is not adopting the exception for residents of counties with high unemployment. New York is not planning to adopt the exception for individuals traveling outside their community for medical care. Twelve states had not made a decision.
Collecting New Data and Data Matching
Collecting New Information at Application and Renewal
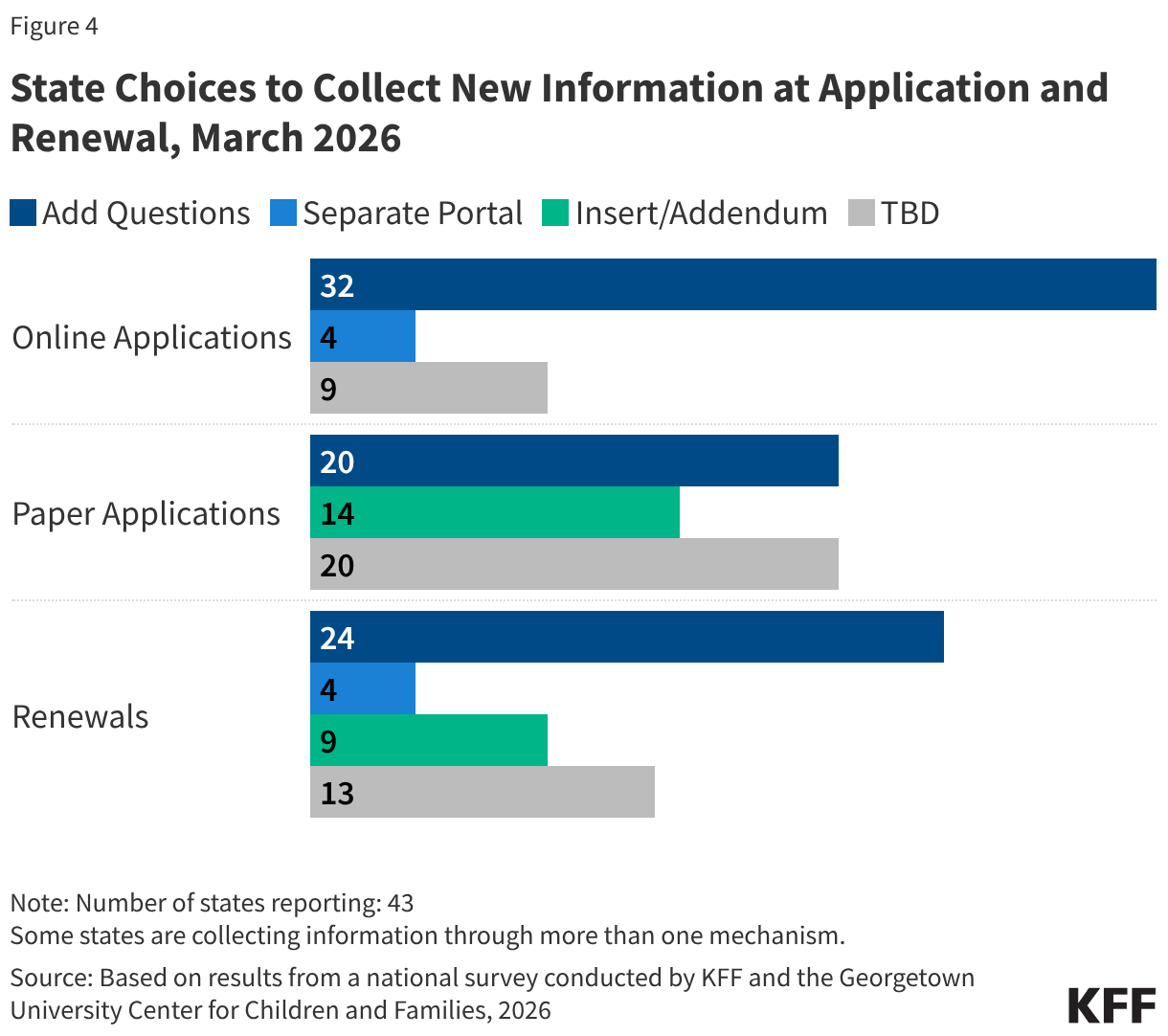
Most states will be adding new questions to online applications and renewals; however, many states are still considering multiple ways to collect the new information needed to verify compliance with work requirements or exemption status. Most states reported they plan to add new questions to their existing online applications (32 states) and renewals (24 states). Four states said they will create separate portals for online applications and renewals for individuals subject to work requirements, and two of those states are both planning to add new questions and create a separate portal. At the same time, some states were continuing to work through the best ways to collect the needed information and had not yet made final decisions (Figure 4).
States are adding new questions and creating inserts or addendums to paper applications and renewal forms. States are exploring different ways of gathering information on paper applications, including adding new questions (20 states) and developing inserts or addendums (14 states), with 11 states doing both (Figure 4). Nine states indicated they will add an addendum to the renewal. About half of states (20) had not yet made final decisions on how they will collect new data.
Data Matching
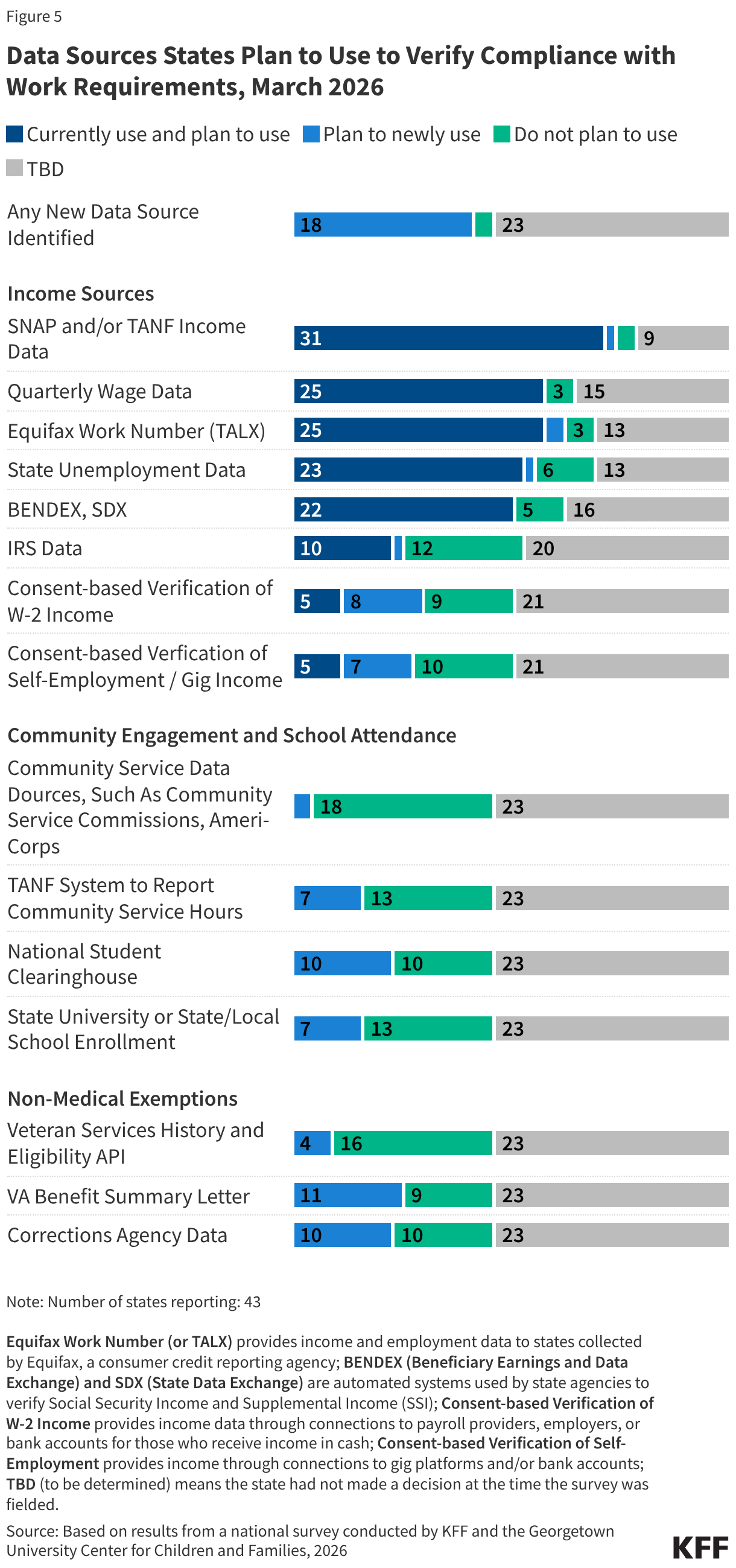
States will continue to use existing data sources to verify income and compliance with work requirements. States are required to use available data from reliable sources to “data match” or check for work compliance or exemption status of individuals to lessen the administrative burden on both enrollees and Medicaid staff. States have long accessed data to verify income to determine Medicaid eligibility, and most states will continue to use income data from existing data sources, including SNAP and/or TANF (31 states), quarterly wage data (25 states), Equifax Work Number (25 states), state unemployment data (23 states), and data from the Beneficiary & Earnings Data Exchange (BENDEX) or State Data Exchange (SDX), which can be accessed directly or through the federal data services hub (22 states) to verify that individuals are meeting the work requirements (Figure 5).
Overall, 18 states had identified new data sources, and 23 states were still deciding whether they have the capacity to access new data sources to verify school attendance, community service, and non-medical exemptions. A priority for states as they implement work requirements is to identify and establish linkages with new data sources, such as student and community service databases and data on veterans, to increase the share of applicants and enrollees who can be automatically determined as having met the requirements. At the time of the survey, only two states were not planning to establish linkages to new data sources, although Colorado indicated it would explore new data sources after initial implementation (Figure 5). The most frequently cited new data sources to data match individuals who qualify for exemptions other than medical-related exemptions include VA Benefit Summary Letter (11 states), and corrections agency data (10 states). States also plan to access new data sources to enhance their ability to verify compliance with work requirements, school attendance, and community service activities, including the National Student Clearinghouse (10 states); consent-based verification of W-2 payroll income through connections to payroll providers such as ADP, employers, or bank accounts (8 states); consent-based verification of self-employment income through a connection to gig platforms and/or connections to bank accounts (7 states); and the TANF system used to report community service hours (7 states). Most states also plan to use Medicaid claims data and data from managed care plans to verify medical-related exemptions, including medically frail exemptions.
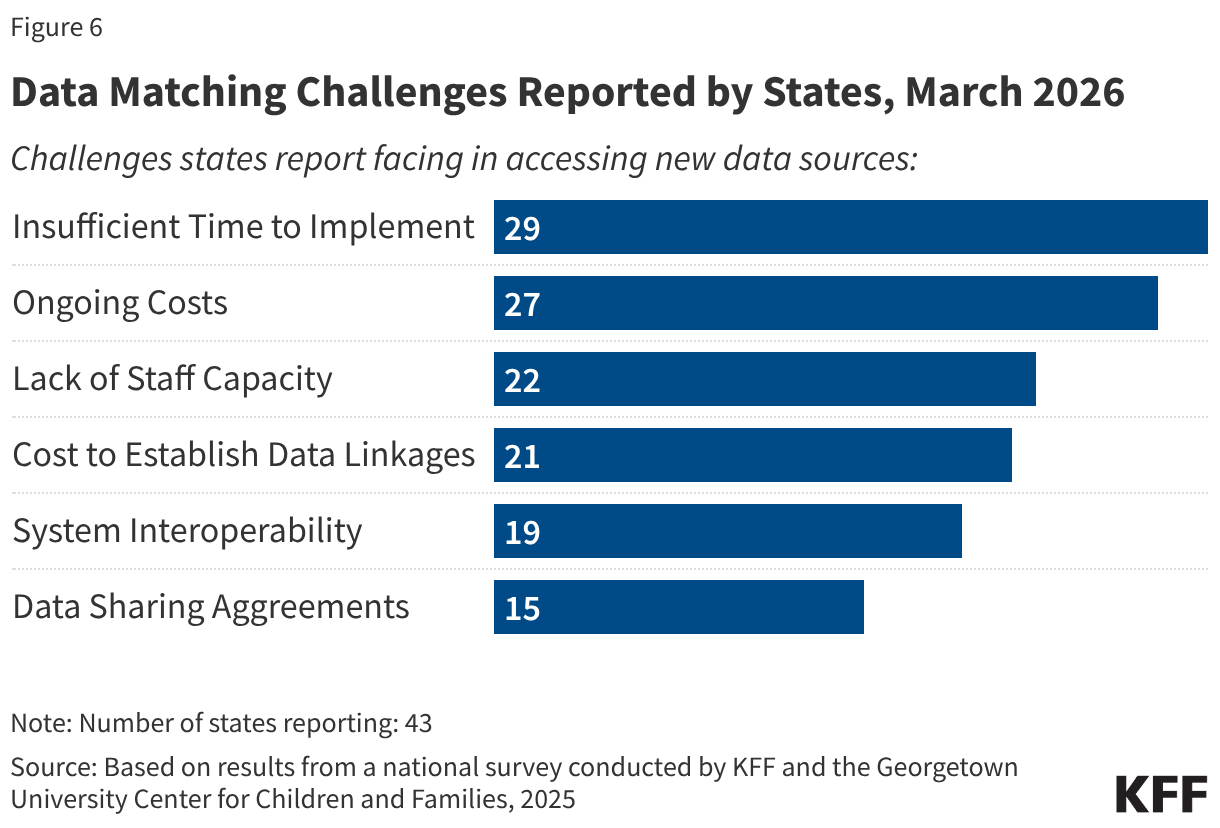
While states are looking to access additional data to increase data matching capacity, they face multiple challenges establishing linkages with new data sources. Facing a very tight implementation timeline, a majority of states (29) cited insufficient time to add new data sources as a major barrier (Figure 6). Costs were also an issue for many states, with 27 states reporting ongoing costs and 21 states reporting the cost to establish data linkages as challenges to accessing new data sources. About half of states indicated a lack of staff capacity (22) and system interoperability (19) were challenges. Fifteen states also cited executing data sharing agreements as another challenge. Only one state said they did not encounter any challenges accessing new data sources while nine states were not yet sure if they would face challenges.
Insights from Focus Group Participants: Data Matching
Focus group participants noted that data matching may not be possible for certain individuals, particularly new applicants who might qualify for a medically-related exemption. While focus group participants estimated that data matching may be able to verify compliance or exemption status of between 60% and 80% of current enrollees who will be subject to work requirements, they expressed concern about being able to find additional data sources or ways of verifying the remaining 20%-40%, in part, because they have little current information on that group.
Specific challenges participants discussed included:
- Data lag issues: For individuals who may be medically frail, participants asserted that claims data will be unavailable for new applicants and likely unavailable for new enrollees at their first six-month renewal. They also discussed other exemptions that may be difficult to verify at application, including American Indian or Alaska Native tribal membership because of the length of time it can take to obtain documentation from tribal offices. One participant also noted that because state wage data are lagged, it may be difficult to verify compliance with work requirements in the month prior to application.
- Community service: Focus group participants expressed uncertainty about verification of community service and said they were waiting on guidance from CMS. They offered examples of some community service data they could potentially access but noted they probably would not be able to get information for most volunteer activities. To try and address this gap, some participants reported developing forms that could be used to document community service activities.
Focus group participants in states that had previously pursued waivers to implement work requirement waivers said that they were building on those efforts to implement the federal work requirements. One state reported being able to “use the same chassis” that was designed for its earlier work requirement waiver, meaning it only had to make slight modifications to align with the new law instead of engaging in a major system redesign. Two states reported having done a good deal of work for their waivers to verify medical frailty, including identifying diagnosis codes and conditions that may qualify. One state reported they were continuing to use a medical frailty identification tool created for their previous waiver.
Medical Frailty and Parent/Caretaker Exemptions
States are waiting on federal guidance on how to define medical frailty but are beginning to operationalize these exemptions. The reconciliation law requires states to exempt from work requirements individuals who are medically frail and specifies medically frail individuals as those who are blind or disabled, have a physical, intellectual, or developmental disability, have a substance use disorder or a “disabling” mental disorder, and those with “serious or complex” medical conditions. To implement this exemption, states will need a comprehensive and detailed definition of who qualifies as medically frail. It is expected that CMS will formalize a federal medically frail definition in the guidance it will release by June; however, it is less clear whether CMS will mandate states use the federal definition or give states flexibility to use a state definition that may be more expansive than the federal definition.
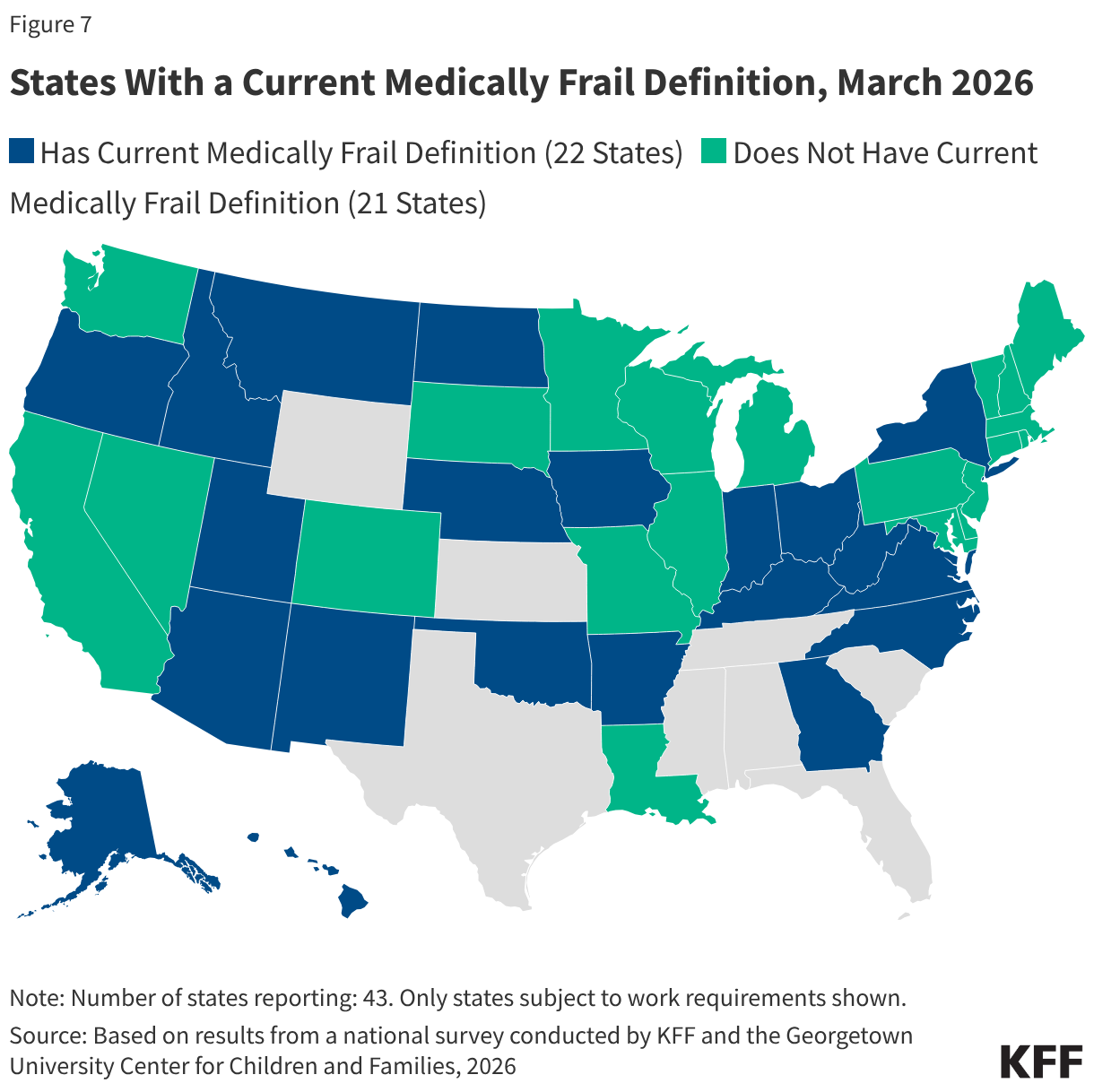
About half of states (22) have a current medical frailty definition, though it is unclear whether these definitions align with the medical frailty provisions in the reconciliation law (Figure 7). States are required to create a medical frailty definition if they provide expansion enrollees a benefit package that is more restrictive than the traditional state plan benefit package. The medical frailty definition in this context is intended to ensure that enrollees who have physical and/or mental health needs but do not qualify for Medicaid based on a disability receive the benefit package that best meets their needs. States may also have previously developed medical frailty definitions when pursuing Medicaid work requirement waivers. If states are given flexibility by CMS to define who is medically frail and exempt from work requirements, six states would prefer to use a state definition, either an existing definition or a new definition, while four states would use a federal definition. Likely reflecting ongoing uncertainty over how much flexibility states will have, the majority of states (33) indicated they had not yet determined what definition they plan to use.
States plan to use a variety of methods to verify medical frailty status, including using data to automate the process where possible. Most states reported plans to use Medicaid claims data (32) to verify medical frailty exemption status, while one state indicated it would not use claims data and the remaining ten states had not yet made a decision (Figure 8). Additionally, ten of the states that reported plans to use claims data have identified or plan to identify both ICD-10 diagnostic codes and CPT service codes to verify medical frailty exemptions. In addition to claims data, states will also use data from other programs, such as enrollment in a behavioral health managed care plan (25 states), managed care utilization or claims data (19 states), and managed care case management data (14 states). In cases where states cannot verify exemption status using Medicaid claims or other data, 30 states indicated they will develop a process to obtain confirmation from a treating provider. Most states (29) also reported wanting to allow applicants and enrollees to self-attest to their medically frail status if verification data are not available. Many states are developing health assessment screeners to collect information to identify medical exemptions, and 11 states said they will use the health screeners to verify medically frail status when data are not available.
Although not asked specifically on the survey, states reported questions related to the parent/caretaker exemption. States said they would like clarity on who can qualify as a caregiver and how to define caregiving. Similar to verification of medical frailty, states are waiting on guidance from CMS as to whether documentation would be needed or whether self-attestation would be acceptable. If verification is required, they also noted uncertainty over what would need to be verified—that the individual is providing care or that the person being cared for has certain health conditions or disabilities or both.
Insight from Focus Groups: Medical Frailty and Parent/Caretaker Exemptions
Focus group participants noted their states were in different stages of identifying data to use to verify medical frailty status and raised other questions related to implementing the medically frail exemption.
- Implementation status: Focus group states differed in how far along they were in the process of exploring claims data and other data that they would be using to verify medical frailty exemptions, with some states already having existing processes and definitions in place and other states only beginning the development process. Participants reported plans to use medical claims data to identify medical frailty, along with screening tools, inpatient treatment participation, information from disability services, health information exchange data, and information provided by medical professionals.
- Existing definitions: Some participants said they were waiting on guidance from CMS that would impact their ability to use existing medically frail definitions and/or identification tools.
- Self-attestation: Multiple participants noted they were uncertain whether self-attestation could be accepted, especially at application when the state would not yet have claims data that could be used that could be used to verify exemption status.
Focus group participants also had lingering questions on how to operationalize the parent/caretaker exemption. These included how to define “significant relationships” for caregivers of disabled individuals and the required level of disability for the person being cared for. Participants offered examples of caregiving situations, such as grandparents taking care of grandchildren five days a week or individuals taking care of their elderly or disabled parents on a part-time basis and wondered whether those relationships would qualify as “significant.”
Vendors, Artificial Intelligence, and Workforce
Vendor Contracts for System Upgrades
Most states reported that they will contract with existing vendors to make the necessary changes to eligibility systems due to the short timeline for implementing work requirements. The short implementation timeline to implement work requirements limits states’ abilities to contract with new vendors because RFP processes to select new vendors are typically too long to meet the January 2027 deadline. In addition, in many states there is a short window for submitting budget requests and getting them approved by state legislatures. Of the 30 states that reported plans to contract with existing vendors, Deloitte is the existing vendor for over half (16 states). No state said it was planning to forgo working with an existing vendor to contract with a new one; however, six states reported plans to use both existing and new vendors.
Insight from Focus Groups: Vendor Contracting
Echoing the survey findings, focus group participants said they will work with existing vendors, but they also discussed hopes for specific tools to ease administrative burden on eligibility staff, while expressing concerns with untested products from new vendors. Focus group participants confirmed that lengthy procurement processes and budget constraints limit their ability to explore contracting with new vendors. One state noted that due to a tight budget situation, getting additional funds has been a challenge, so they are leveraging time built into vendor contracts for system fixes and enhancements.
- New vendor concerns: Participants also noted that while many vendors have presented new solutions to facilitate implementation of work requirements, many of these products are untested. They expressed concerns that, if adopted, these tools might not function as intended or might take too many resources to integrate with existing systems. Although focus group participants did not discuss artificial intelligence (AI) specifically, many of the tools being developed by new vendors use AI in some way. One state made the point that the solutions pitched by vendors are unlikely to be able to provide data to verify the status of individuals the states expect to have the most challenges with, such as gig workers, medically frail individuals, and individuals experiencing homelessness.
- Desire for tools to streamline the verification process: Although none of the focus group states were contracting with new vendors at the time of the focus groups, several states described the types of tools they would like to adopt to reduce administrative burden. One state said they were looking for a vendor to enable them to use claims data and other data not currently in their eligibility system to flag individuals for exemption or compliance. Another state said they were hoping to find a vendor that could assess compliance verifications to reduce caseworker workload.
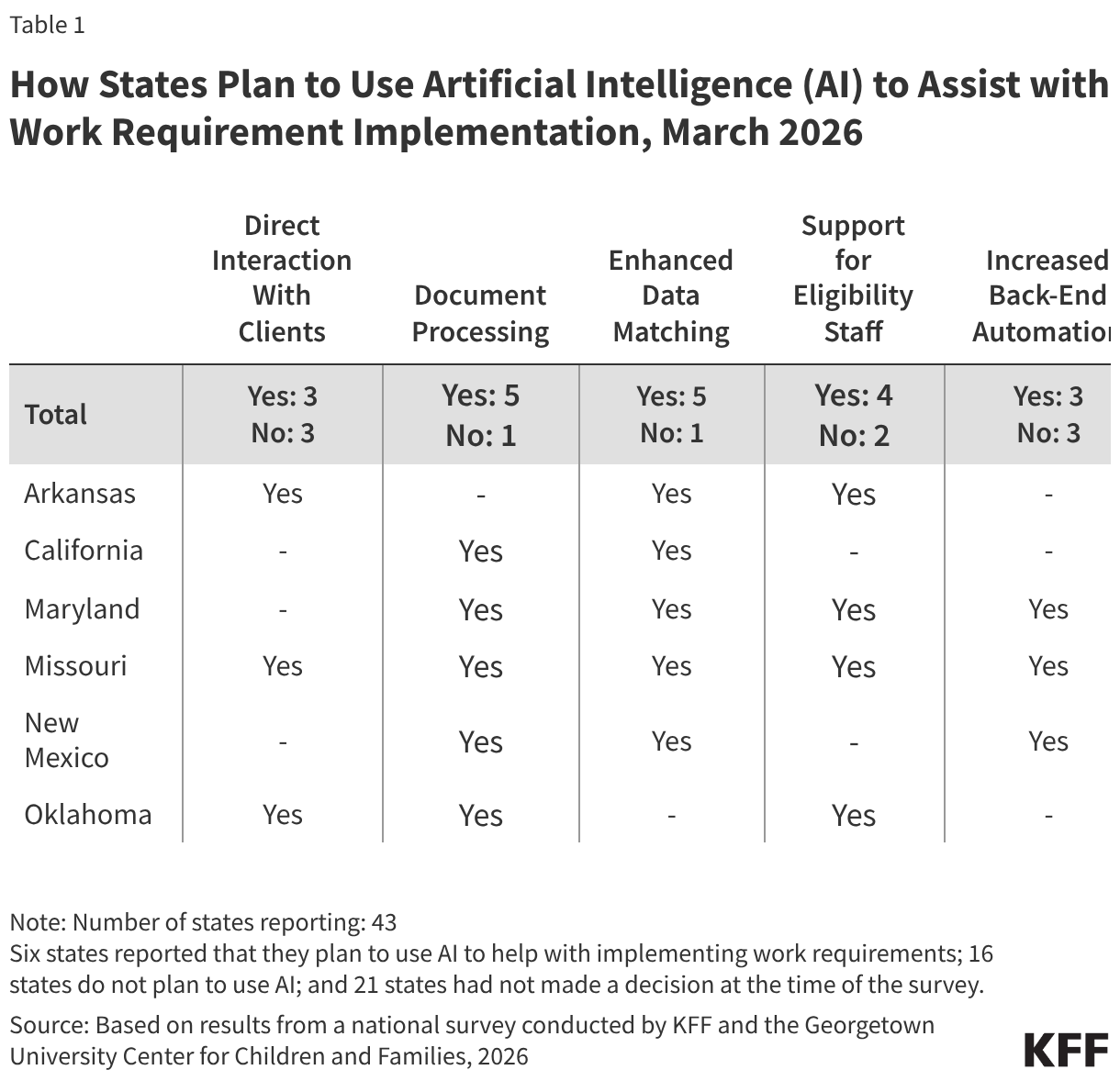
A small number of states reported they are using artificial intelligence (AI) to assist with implementing work requirements. Six states (Arkansas, California, Maryland, Missouri, New Mexico, and Oklahoma) reported plans to use AI, with another 21 states reporting they had not made a final decision (Table 1). Five of the six states said they intend to use AI to assist with processing documents and to enhance data matching capabilities. Four states will rely on AI to provide support for eligibility staff while three states will deploy AI to increase back-end automation. To facilitate the use of claims data for identifying individuals who are medically frail, two states will use AI to review claims or utilization data for specific ICD-10 or CPT codes. In three states, AI will interact directly with clients, likely to assist with identifying and uploading verification documents.
Workforce Capacity
Fourteen states said they plan to take action to increase the capacity of eligibility staff to implement work requirements, although many states had not yet made a decision. Among the states that plan to boost staff capacity, the strategies they will adopt include: hiring new eligibility workers (9 states); hiring contractors (7 states); and approving overtime (6 states). Nine states had no plans to increase staff capacity while 20 states had not made a final decision. States may be limited in their ability to increase eligibility staff due to budgetary constraints or hiring challenges.
Insights from Focus Groups: Workforce Capacity
Focus group participants described workforce capacity limitations that were affecting implementation, including the inability to add new data sources for verification. Focus group participants acknowledged that without additional automation, verification requirements would likely increase the manual processing workload for caseworkers. At the same time, some participants also noted that existing staff capacity limitations would keep them from implementing system changes to access new data sources that could increase automation of verifying compliance with work requirements or exemption status. One participant said that due to staffing limitations, they expect to mainly rely on current data sources initially but would evaluate adding new data sources post implementation. Another participant in a state where the Medicaid eligibility system is integrated with SNAP described having to coordinate and stagger changes to both programs to balance staff capacity.
Guidance Needed from CMS
States cited the need for timely guidance from CMS on a range of issues, particularly how to define certain exemptions and community engagement activities and what verification methods can be used. States most frequently mentioned a desire for additional guidance on how to define medical frailty, with some states asking specifically for clarity on whether they will have flexibility to use their own definitions. States also want direction on what qualifies as community service, how to calculate half-time school attendance, and what is considered a “significant relationship” to qualify for the caregiver exemption. States also said they want guidance on verification requirements and acceptable verification methods. Specifically, they want to know what sources can be used for verification, whether self-attestation will be allowed if other sources are not available, and the length of time verification of exemptions remain valid. In addition, states had questions related to eligibility transitions and changes in circumstances between renewal periods, particularly when individuals moving into the expansion group need to meet the work requirements if they transition between renewal periods.
Insights from Focus Groups: Guidance Needed from CMS
Although focus group participants reported waiting on guidance from CMS on multiple issues, the tight implementation timeline was forcing them to make key policy decisions and move forward with systems changes before receiving formal guidance. Multiple participants explained that because of the time required to make systems changes, they were having to move forward with decisions before receiving guidance from CMS. Participants acknowledged that there were risks to making systems changes based on working assumptions of policy before guidance has been finalized, and many said they were developing contingency plans for making adjustments if federal policies are different from what they expected. Participants also noted that making changes after starting development increases costs and time.
Beyond the issues described above, focus group participants are also seeking guidance on verifying income and look back periods.
- Income verification: One participant said they were waiting for a decision from CMS on whether they could use additional sources such as unearned income to make determinations for applicants. Multiple participants said they were hoping for additional guidance related to what flexibility they could have with interpreting income data, such as making assumptions using historical data and being able to average income over months.
- Look-back periods: Multiple participants said additional guidance about how to handle look-back periods would be helpful. In particular, participants expressed concern about how to handle individuals who were compliant in the month in which they were applying for coverage but were not compliant in the prior month. While participants acknowledged these individuals would not meet the work requirements for enrollment in the month in which they were applying, participants wanted clarity on whether they could enroll these individuals starting the next month without a new application.
Focus group participants also noted the challenges of building systems to implement work requirements in the absence of guidance on the new requirements and penalties for improper payment errors. Participants said the new penalties are a factor they are considering as they program system changes. Participants also said that they may be more cautious when considering what data they are accepting or changes they are making due to concerns about the penalties and what an auditable attestation will look like.