One source of the 2025 reconciliation law’s Medicaid cuts is a 10-year moratorium on implementation or enforcement of certain provisions in two rules finalized by the Biden administration that would have reduced administrative burdens to make it easier for people to enroll in and maintain Medicaid and CHIP coverage. Many of those changes were intended to streamline Medicaid eligibility and renewal processes for non-MAGI enrollees. Some of the provisions in the rules were excluded from the delay, including those that have already taken effect. While the law prohibits the Secretary of the Department of Health and Human Services (HHS) from implementing or enforcing provisions subject to the delay until October 1, 2034, it does not prohibit states from implementing the changes. In some cases, states have already made the changes required by the rules, either in anticipation of implementation of the new requirements or as part of other efforts to streamline or simplify processes. It is unknown whether states will maintain the changes now that federal requirements have been delayed or whether additional states will adopt similar changes before the requirements take effect.
The law pauses implementation of provisions that align application and renewal policies for individuals eligible through MAGI and non-MAGI pathways. The Affordable Care Act (ACA) created consistent, streamlined application and renewal policies for individuals who qualify for Medicaid based on modified adjusted gross income (MAGI), but those policies were not extended to people eligible for Medicaid through non-MAGI pathways. Provisions of the delayed rule would require states to extend some of the streamlined MAGI procedures to non-MAGI processes. These include eliminating in-person interviews as part of eligibility determinations, requiring states to renew coverage no more frequently than every 12 months, requiring that non-MAGI applications and forms be accepted through the same modalities as MAGI applications and forms, and requiring states to send pre-populated renewal forms to non-MAGI enrollees whose ongoing eligibility cannot be confirmed through available data sources.
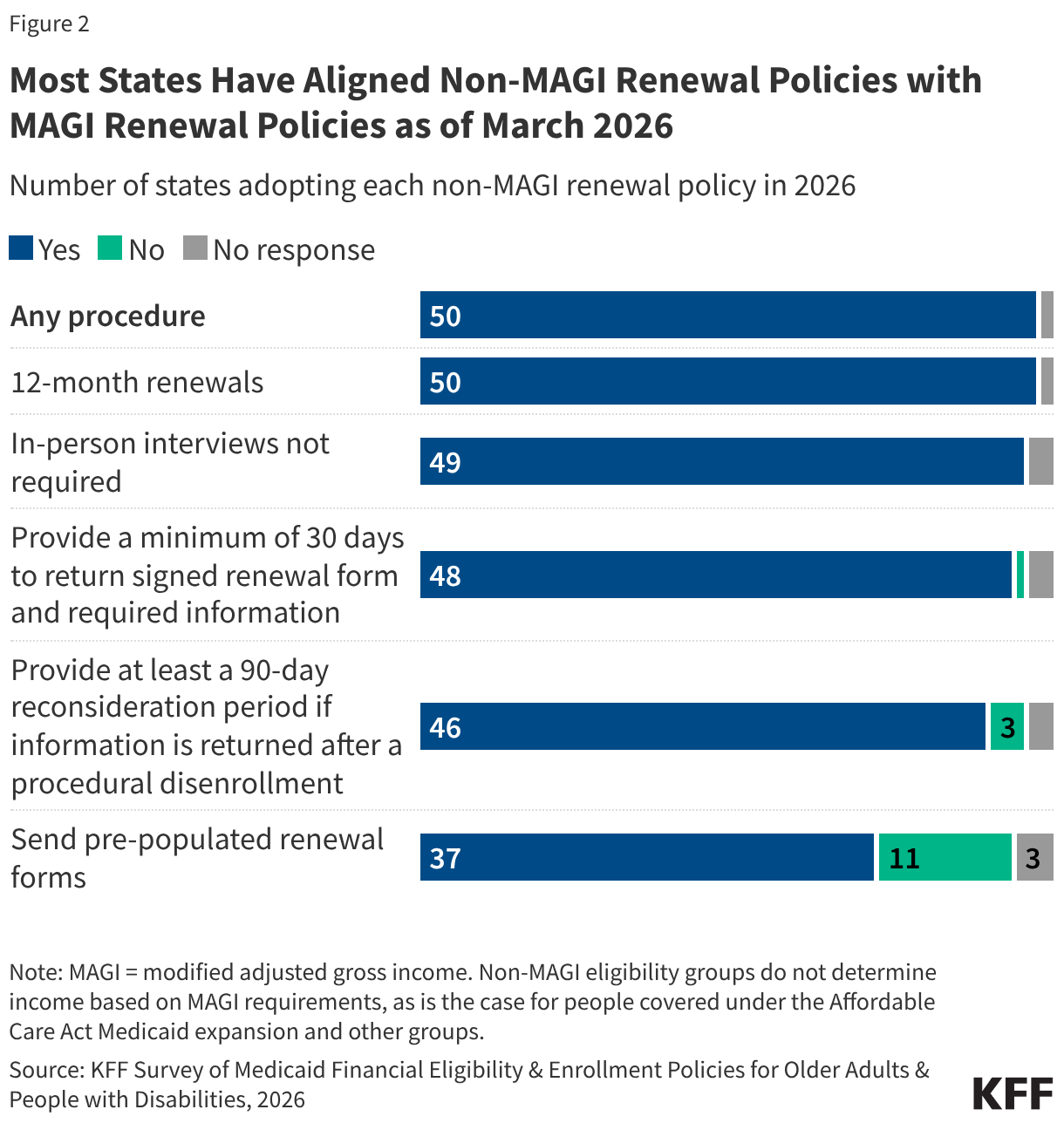
Many of the application renewal policies for non-MAGI eligibility pathways have already been implemented by nearly all states despite the pause in the federal rule (Figure 2). All responding states align at least some renewal policies for non-MAGI populations with those for most MAGI populations (Appendix Table 8). The most widely adopted changes include renewing eligibility only once every 12 months (all responding states), no longer requiring in-person interviews (all responding states), and providing enrollees with at least 30 days to sign and return required paperwork for renewals (all responding states except for Minnesota). The least widely adopted changes include providing a reconsideration period of at least 90 days after a procedural disenrollment (all responding states except for Alaska, New Mexico, and Washington) and using pre-populated renewal forms (37 states).
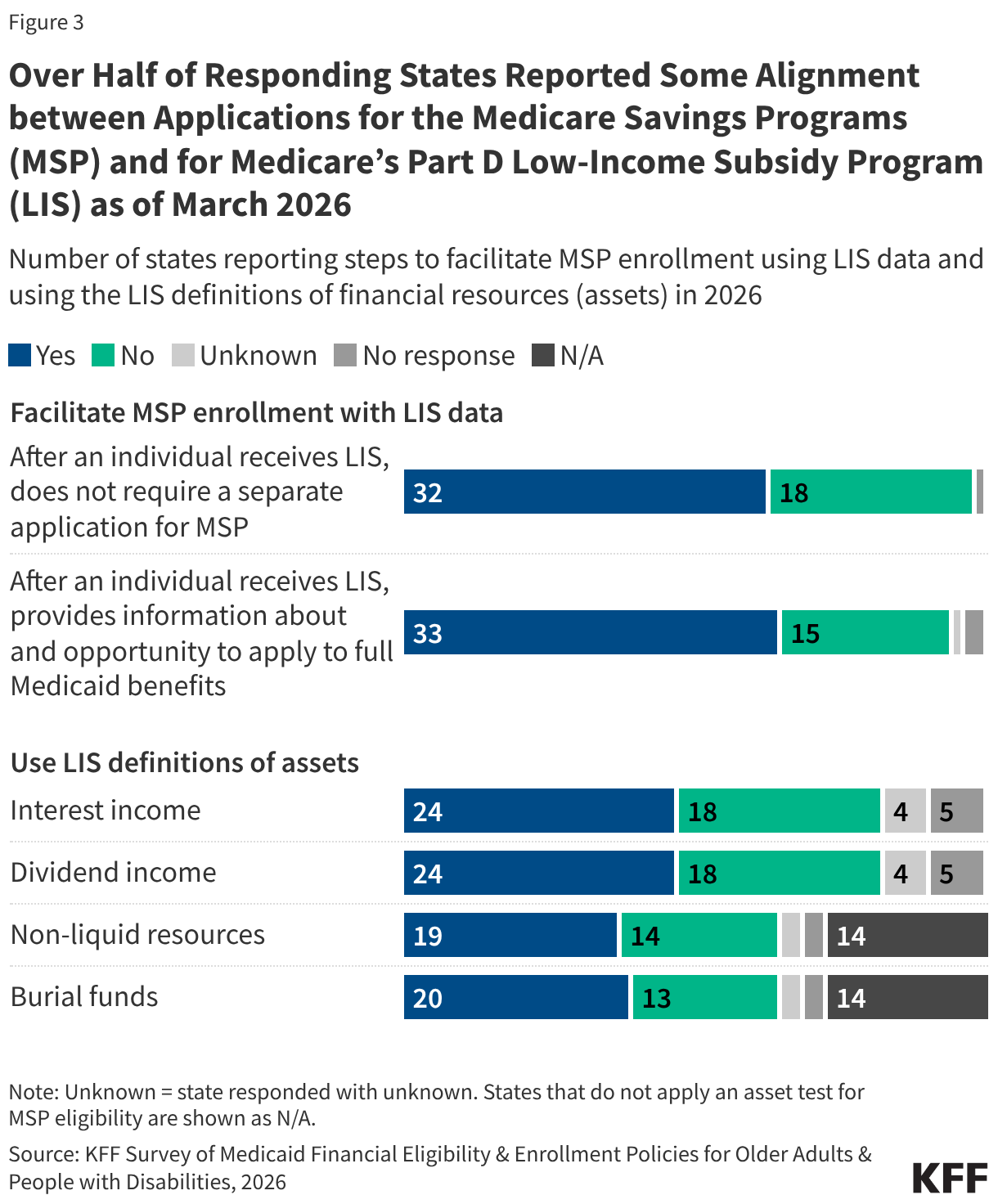
The law delays several provisions that facilitate enrollment in the Medicare Savings Programs, but those changes have already been implemented by over half of states (Figure 3). Specifically, the delayed rule aimed to facilitate enrollment into the Medicare Savings Programs using information from the Medicare Part D Low-Income Subsidy (LIS) data and encourage states to use the Medicare Part D LIS definitions of financial eligibility. The Medicare Part D Low-Income Subsidy (LIS) is a program that helps Medicare beneficiaries pay for prescription drugs. A larger number of Medicare beneficiaries are enrolled in the Medicare Part D LIS than in the Medicare Savings Programs. Fewer states responded to these survey questions than is the case for other survey questions, and several states reported that they did not know the answer to questions about aligning definitions of financial resources. Even so, most responding states reported using the LIS data to enroll people into the Medicare Savings Programs without a separate application, and over half of states reported using the same definitions of specific types of financial resources (Appendix Table 9). The District of Columbia noted it was in the process of implementing LIS data to initiate Medicare Savings Program applications, but the 2025 budget reconciliation law halted those efforts.
This work was supported in part by Arnold Ventures. KFF maintains full editorial control over all of its policy analysis, polling, and journalism activities.